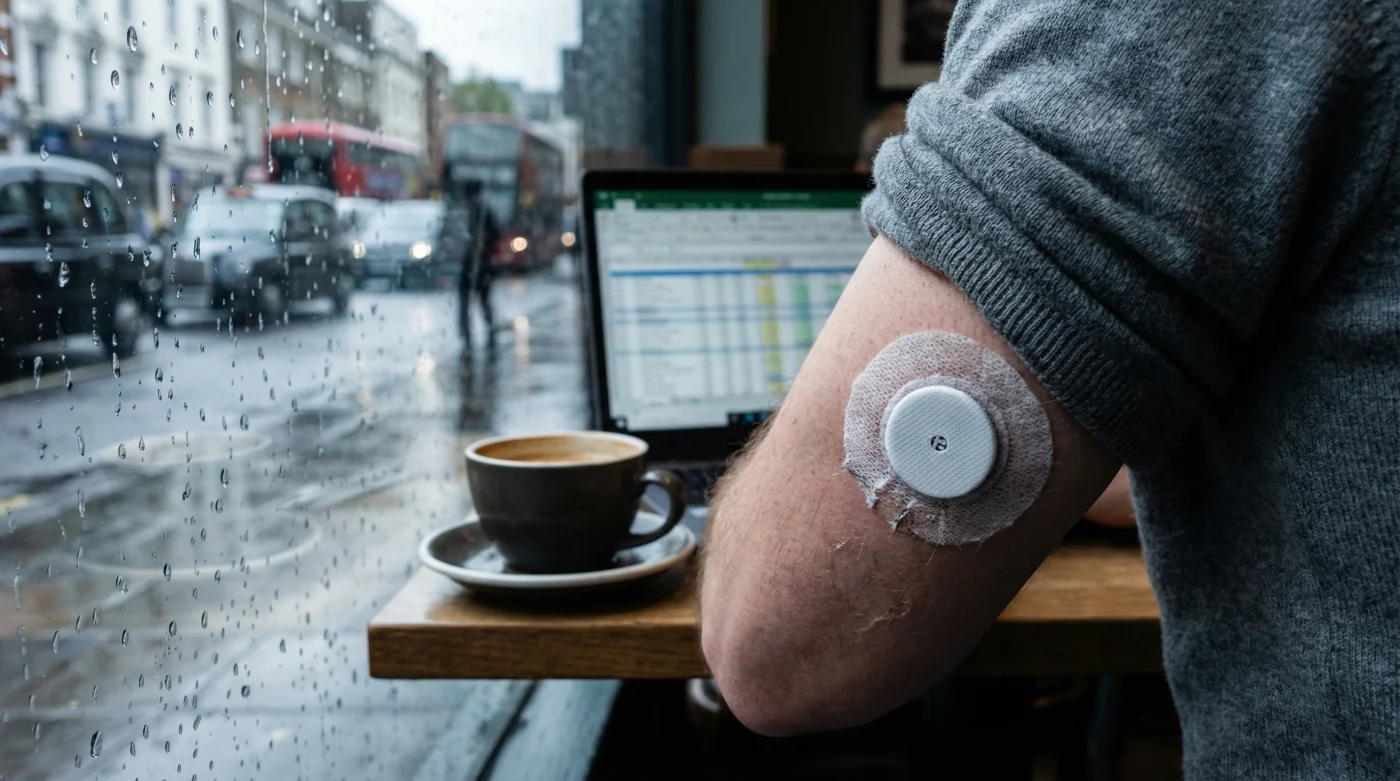
It starts with the dreaded 3 pm slump—that heavy, unavoidable brain fog that sends you reaching for a packet of Hobnobs or a third cup of tea. But for a rapidly growing cohort across the UK, the solution is no longer found in the kettle or the biscuit tin; it is stuck to the back of their arm. A quiet revolution is taking place in offices, gyms, and homes from London to Edinburgh, where medical-grade technology is being repurposed for peak performance, fundamentally changing how we understand energy.
The technology in question—Continuous Glucose Monitors (CGMs)—was once strictly the preserve of those managing diabetes. Now, it has become the ultimate status symbol for the health-conscious, promising to unlock the secrets of metabolic health. By tracking blood sugar spikes in real-time, Britons are discovering that their "healthy" morning porridge might be the very thing sabotaging their productivity, leading to a surge in private sensor sales that is currently shattering industry records.
The Metabolic Awakening: Why The UK Is Obsessed
For decades, we have been told that weight management and energy levels are simply a matter of "calories in, calories out." However, the explosion of blood sugar technology has revealed a far more complex picture. This is not just a trend; it is a fundamental shift in our understanding of biology. The focus has moved from simple weight loss to metabolic flexibility—the body’s ability to switch efficiently between burning fuel sources.
"What we are seeing is the democratisation of biological data. People are realising that a sandwich from a High Street chain affects their biochemistry differently than it affects their colleague’s. That personalisation is the new standard." — Dr. Sarah Jenkins, Metabolic Health Researcher.
The premise is simple yet terrifyingly effective: instant accountability. When you can see a graphical spike in your glucose levels minutes after eating a bagel, the immediate bio-feedback creates a behavioural change that diet books simply cannot replicate. This has led to a boom in apps that pair with these sensors, categorising food not by "good" or "bad," but by how your specific biology responds to it.
Beyond the Finger Prick: The Tech Explained
Unlike the smartwatches that track your steps or heart rate via optical sensors, CGMs are invasive, albeit minimally. They use a tiny filament inserted just under the skin to measure interstitial fluid glucose levels. This provides a dynamic film of your metabolic day, rather than the single snapshot provided by traditional finger-prick tests.
- Put your phone in the drawer before starting the first episode of Vladimir
- Why the 2026 inflammation conversation is the smartest move for your youth
- Neither the school nor the GP can fix the assessment wait times
- Stop ignoring that mild chest fluttering and visit a 2026 heart clinic
- NHS confirms the real reason for the 2026 school breakfast club rollout
- Glycaemic Variability: How much your blood sugar swings up and down. Less variability generally equals better energy and longevity.
- The Post-Prandial Spike: How high your glucose goes after a meal. The goal is a gentle hill, not a mountain peak.
- Fasting Glucose: Your baseline levels while you sleep or before eating.
Comparison: Old School vs. The New Standard
To understand why this wearable tech is breaking records, one must look at how it compares to previous methods of tracking health data.
| Feature | Traditional Finger Prick | Optical Smart Watch | Continuous Glucose Monitor (CGM) |
|---|---|---|---|
| Data Frequency | Single Snapshot | Continuous (Heart Rate/O2) | Every 1-5 Minutes (24/7) |
| Accuracy | High (Blood) | Variable (Optical) | High (Interstitial Fluid) |
| Pain Level | Sharp pinch every time | None | One-time application pinch |
| Cost | Low (£) | Medium (££) | High Subscription (£££) |
The ‘Afternoon Slump’ Connection
The primary driver for the non-diabetic market in the UK is energy management. The phenomenon known as the "afternoon slump" is often directly correlated to reactive hypoglycaemia—a crash in blood sugar following a large spike. By flattening these curves, users report stable energy without the need for caffeine. It turns out that stabilising glucose does what five espressos cannot: it keeps the brain fuelled steadily.
However, the trend is not without its critics. Some NHS doctors worry that the "worried well" are obsessing over normal physiological responses. It is normal for blood sugar to rise after eating. The danger lies in misinterpreted data leading to unnecessary dietary restrictions, such as cutting out healthy fruits or whole grains solely to avoid a line on a graph going up.
Frequently Asked Questions
Does applying the sensor hurt?
Most users describe the application as painless or feeling like a very light flick. The device uses a spring-loaded applicator to insert a hair-thin filament, and once it is on, you typically cannot feel it.
Is this available on the NHS?
Generally, no. Unless you have Type 1 diabetes or specific Type 2 conditions requiring intensive insulin management, the NHS does not fund CGMs. The trend discussed here is driven by the private market, with subscriptions costing between £40 and £150 per month.
Can a smart watch measure glucose without a needle?
Not yet accurately. While major tech giants are racing to develop non-invasive optical glucose monitoring, the technology is not yet reliable enough for medical or serious health optimisation standards. For now, the filament sensor remains the gold standard.
Will this really help me lose weight?
It can be a powerful tool. By seeing which foods cause massive insulin spikes (which can promote fat storage), users often naturally gravitate towards a diet that supports a leaner composition, though the sensor itself does not burn fat.
Read More